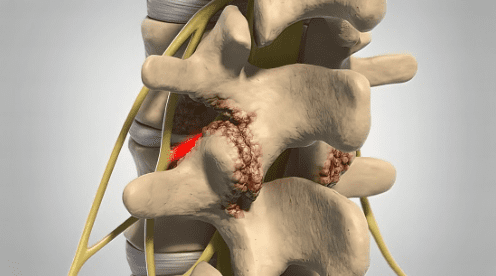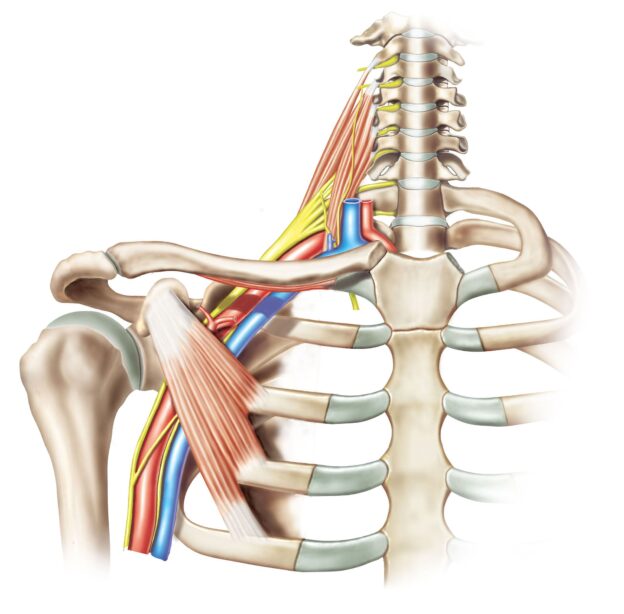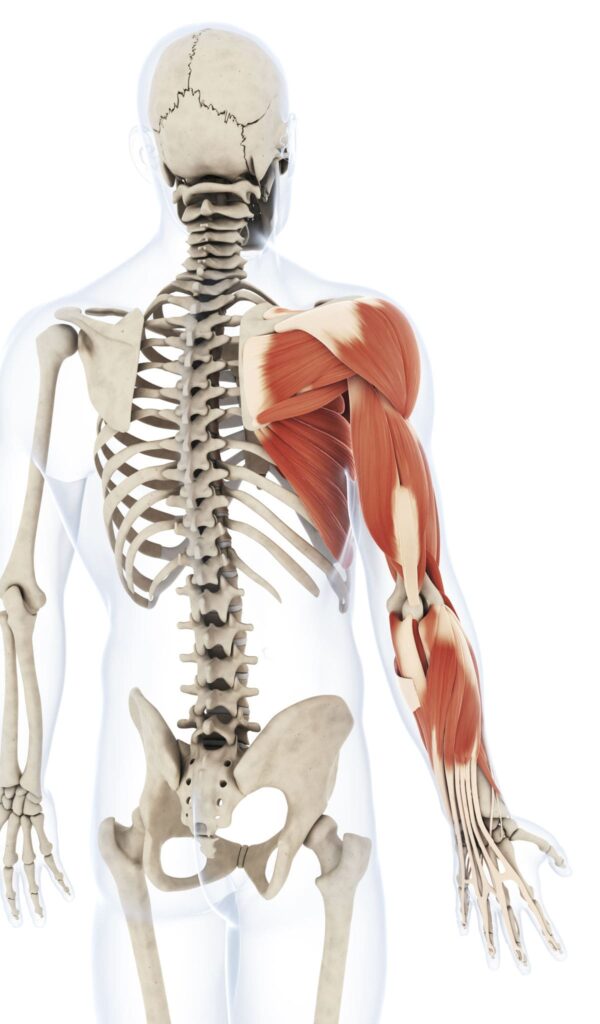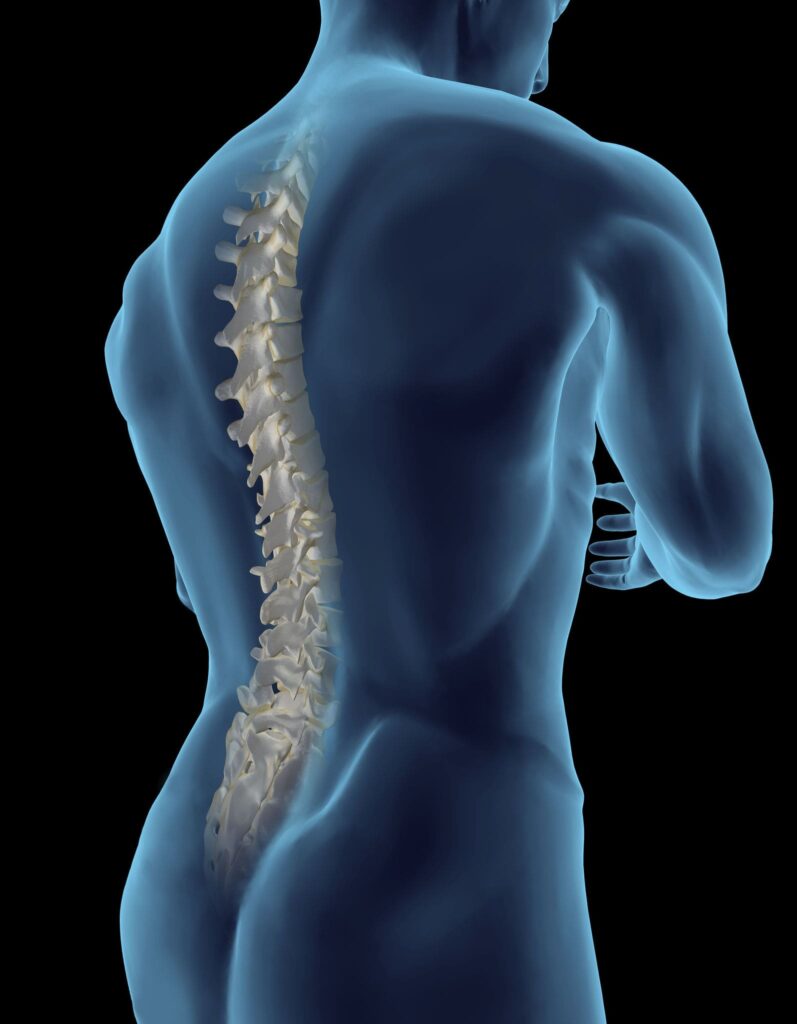
The thoracic spine is the middle section of the spine, and it is made up of 12 vertebrae (T1 to T12). It is located just behind your chest. The pain in the thoracic spine can be caused due to several reasons. However, not all reasons require surgical treatment. If you are scheduled for thoracic spine surgery, it is important that you understand what to expect. This article will provide you with all the information you need. We will discuss the procedure itself, as well as the risks and recovery process. This information will help you feel confident and prepared before your surgery!
Why is Thoracic Spine Surgery Performed?
It is typically performed to treat conditions that cause pain or compression in the middle area of the spine. Some common reasons for thoracic spine surgery include:
- Herniated Disc
- Degenerative Disc Disease
- Spinal Stenosis
- Spondylolisthesis
Preop Guidelines
Successful surgery and recovery entail strict adherence to pre-op guidelines. The guidelines are very much similar to other spine surgeries.
- You will need to fast for at least six hours before the time of your surgery.
- Avoid drinking alcohol and smoking as they can hinder the effect of anesthesia.
- Blood thinners must also be avoided to prevent excessive blood loss during surgery.
- Provide accurate answers in pre-surgery meetings regarding your medical history, allergies, lifestyle choices, etc.
- Other than these general guidelines, there are 5 perioperative spine assessments identified by the Congress of Neurological Surgeons; Osteoporosis assessments, nutrition assessments, pulmonary evaluation and optimization, opioid evaluation, and surgical risk assessment.
Procedure for Thoracic Spine Surgery
The thoracic spine surgery itself is fairly complex, and it usually takes several hours to complete. During the surgery, your surgeon will access the thoracic spine through an incision in your back. Once they have access to the spine, they will remove any damaged or diseased tissue. In some cases, they may also need to fuse together some of the vertebrae to stabilize the spine. The specific type of thoracic spine surgery that is required will depend on the underlying condition being treated.
After your surgery, you will be closely monitored in the hospital for any complications. Once you are discharged, you will need to take it easy and avoid strenuous activity for at least six weeks. You will also need to follow up with your surgeon periodically to make sure that your recovery is progressing as planned.
Types of Thoracic Spine Surgery
There are different types of thoracic spine surgery, each designed to address a specific problem or condition. The most common type is called the laminectomy. This procedure involves removing the lamina, which is the bony plate that covers the spinal cord. Laminectomies are often performed to relieve pressure on the spinal cord or nerves.
Other types of thoracic spine surgery include;
Spinal fusion – This procedure involves joining two or more vertebrae together. This is often done to stabilize the spine and relieve pain.
Decompression – This procedure involves relieving pressure on the spinal cord or nerves by removing bone or other tissues.
Disc replacement – This procedure involves removing a damaged disc and replacing it with an artificial disc.
Your surgeon will choose the appropriate procedure after evaluating your medical condition.
Risks Involved in Thoracic Spine Surgery
Most spine surgeries are safe and do not lead to any major medical complications. However, different people have different risk vulnerabilities. There are several factors that determine this risk. For example, medical history, overall health condition, age, coexisting medical conditions, and Osteoporosis. Following are some of the common risks that need to be considered when undergoing thoracic spine surgery;
- Surgical site infection
- Nerve damage
- Injury to the spinal cord (rare)
- Blood clots
- Spinal fluid leak
- Spinal headache after surgery
It is important to discuss all of the potential risks and side effects of thoracic spine surgery with your surgeon before having the procedure. This will help you to make an informed decision about whether or not this type of surgery is right for you.
Recovery after Thoracic Spine Surgery

After undergoing thoracic spine surgery, it is important to follow your surgeon’s instructions for a successful recovery. Depending on the type of surgery you had, you may be able to go home the same day or may need to stay in the hospital for a few days.
In either case, you will need to take it easy for the first few days or weeks and avoid any strenuous activity. You may also need to wear a brace to support your spine as it heals. Physical therapy can also be helpful in regaining strength and mobility.
Most people are able to return to their normal activities within a few months, although some may experience ongoing pain or other issues. Follow-up appointments with your surgeon are important to ensure that your recovery is on track. Working with a professional physiotherapist for smooth and fast recovery is also recommended.
Choosing the right surgeon can make things a lot easier for you in terms of getting smooth treatment and post-surgical assistance. Before you finalize the surgeon for your treatment, spend some time researching different doctors. Shortlist doctors based on their experience and patient ratings. For this purpose, you can check websites like Yelp and Healthgrades.
See a Spine Surgeon in Los Angeles
Looking for a spine surgeon in Los Angeles for thoracic spine surgery? Schedule an appointment with Moksha Ranasinghe MD at Southern California Brain & Spine Surgery. She has been treating patients with spine problems for more than 20 years. For appointment scheduling, you can call (213)-369 4583 or fill out the contact form available on our website.