
Complete Guide: How to Treat Brachial Plexus Injury with Conservative and Surgical Options
Brachial plexus injuries affect the complex nerve network connecting the spinal cord to the shoulder, arm, and hand. Understanding how to treat brachial plexus injury effectively requires expert evaluation, appropriate timing, and comprehensive care from specialists experienced in peripheral nerve reconstruction. At Southern California Brain and Spine Surgery, Dr. Moksha Ranasinghe provides advanced treatment for brachial plexus injuries using both conservative and surgical approaches.
This comprehensive guide explains everything patients need to know about how to treat brachial plexus injury, including when conservative care works, surgical options, timing considerations, and recovery expectations.
Understanding Brachial Plexus Injuries
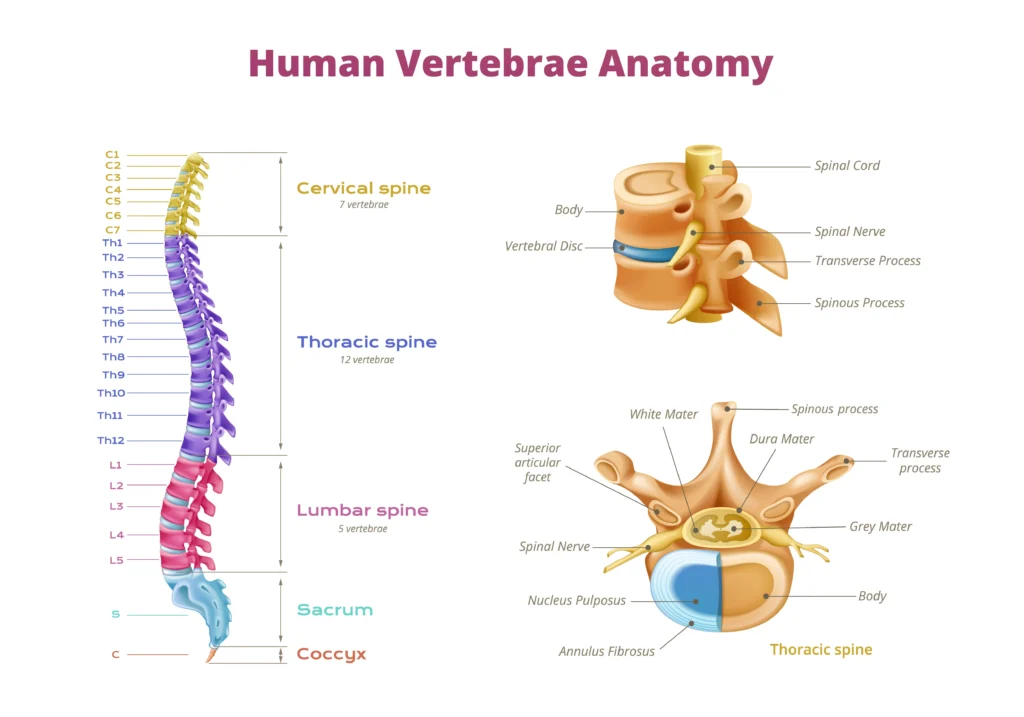
The brachial plexus is a network of nerves arising from spinal cord segments C5, C6, C7, C8, and T1 in the neck. These nerves branch and intertwine before extending down the shoulder and arm, controlling all movement and sensation in the upper extremity. When trauma damages this nerve network, the resulting brachial plexus injury can cause devastating loss of arm and hand function.
Brachial plexus injuries most commonly occur from motor vehicle accidents, motorcycle crashes, sports injuries, or difficult childbirth. The severity ranges from mild stretching (neurapraxia) that heals spontaneously to complete nerve root avulsion requiring complex surgical reconstruction. Understanding how to treat brachial plexus injury depends critically on accurate diagnosis of injury type and severity.
As a top spine surgeon in Los Angeles specializing in peripheral nerve reconstruction, Dr. Ranasinghe emphasizes that early evaluation and appropriate treatment timing make the difference between good functional recovery and permanent disability.
Types of Brachial Plexus Injuries
Learning how to treat brachial plexus injury begins with understanding the different injury types:
Neurapraxia (Stretch Injury) The mildest form occurs when nerves are stretched but not torn. The nerve covering (myelin sheath) is damaged but the nerve fibers remain intact. These injuries typically heal spontaneously within weeks to months without surgery. Recovery rates approach 90-100% with conservative treatment.
Axonotmesis (Nerve Fiber Damage) More severe stretching damages the nerve fibers themselves while the nerve sheath remains partially intact. These injuries may recover spontaneously or may require surgical intervention depending on the extent of damage. Recovery potential varies based on severity.
Neurotmesis (Complete Nerve Disruption) The most severe injury involves complete tearing of nerve fibers and surrounding tissue. These injuries cannot heal without surgical intervention. The nerve ends must be surgically reconnected or bypassed through nerve transfer procedures.
Root Avulsion The most devastating injury occurs when nerve roots tear away from the spinal cord itself. These injuries require the most complex surgical reconstruction and have the most limited recovery potential, though modern nerve transfer techniques can restore some function.
Conservative Treatment: How to Treat Brachial Plexus Injury Without Surgery
Many patients wonder how to treat brachial plexus injury without surgery. Mild to moderate injuries often respond well to conservative care, particularly when evaluation by a top spine surgeon in Los Angeles confirms good recovery potential.
Physical Therapy and Rehabilitation
Physical therapy forms the foundation of conservative brachial plexus injury treatment. Therapy goals include preventing joint stiffness, maintaining muscle flexibility, preserving range of motion, and gradually rebuilding strength as nerve function returns. Therapists design customized exercise programs addressing each patient’s specific functional deficits.
Research demonstrates that patients beginning physical therapy early achieve better overall outcomes whether or not surgery eventually becomes necessary. Therapy preserves joint mobility and prevents contractures (tendon shortening from lack of use) that can limit functional recovery even after successful nerve repair.
Pain Management
Brachial plexus injuries frequently cause severe neuropathic pain – burning, shooting, or crushing sensations in the affected arm. Pain management strategies include medications (gabapentin, pregabalin, duloxetine for nerve pain), topical creams reducing local pain, nerve blocks providing temporary relief, and in severe cases, interventional pain procedures.
Some patients develop deafferentation pain after nerve root avulsion, an especially challenging pain syndrome requiring multidisciplinary pain management including medications, physical therapy, psychological support, and sometimes specialized procedures.
Bracing and Orthotics
Braces help prevent contractures while waiting for nerve recovery. Shoulder slings support the arm and reduce joint strain. Wrist and hand splints maintain functional positions preventing permanent deformities. The top spine surgeons in Los Angeles coordinate with skilled orthotists ensuring proper brace fit and function.
Monitoring for Recovery
During conservative treatment, specialists monitor for signs of nerve regeneration including return of sensation, muscle twitching (fasciculations indicating nerve reconnection), gradual strength improvement, and reduced pain. Electromyography (EMG) and nerve conduction studies performed 6-8 weeks post-injury and repeated at intervals document objective recovery progress.

When Surgery Becomes Necessary: Advanced Treatment Options
Understanding how to treat brachial plexus injury surgically becomes critical when conservative care proves insufficient. The top spine surgeons in Los Angeles recommend surgery when nerves fail to recover spontaneously, progressive functional deficits develop, complete nerve disruption is confirmed, or quality of life is severely impacted.
Critical Timing Consideration: Surgery is most effective when performed 3-6 months post-injury for most cases. Earlier surgery risks operating on nerves that would have recovered spontaneously. Delayed surgery beyond 6-12 months allows irreversible muscle atrophy that limits functional recovery even after successful nerve repair.
Nerve Grafting
When nerve ends cannot be directly reconnected due to gap distance, nerve grafting bridges the gap using donor nerves (typically harvested from less critical sensory nerves in the leg). The surgeon removes damaged nerve tissue and connects healthy nerve ends using grafts as bridges for nerve regeneration.
Nerve grafting offers advantages including direct pathway for regeneration and large source of donor axons from intact nerve roots. However, regeneration must occur over long distances (nerve regrows approximately 1mm per day), limiting effectiveness for injuries far from target muscles.
Nerve Transfer (Neurotization)
Modern nerve transfer techniques represent major advances in how to treat brachial plexus injury. Rather than grafting from damaged roots, surgeons transfer nearby working nerves to the paralyzed muscles. This creates shorter distances for nerve regeneration and bypasses the zone of injury entirely.
Common nerve transfers include transfer of ulnar or median nerve branches to restore biceps function, transfer of spinal accessory nerve to restore shoulder function, and transfer of intercostal nerves to restore various arm functions. As a top spine surgeon in Los Angeles, Dr. Ranasinghe has extensive experience selecting and performing nerve transfers achieving 80-90% success rates for restoring critical functions.
Neurolysis
When scar tissue compresses but hasn’t completely severed nerves, neurolysis (surgical freeing of the nerve from surrounding scar) may restore function. This procedure works best for injuries in continuity where electrical studies suggest some nerve function remains.
Free Functioning Muscle Transfer
For severe injuries where nerve reconstruction cannot restore adequate function, free functioning muscle transfer moves a complete muscle (with its blood supply and nerve) from elsewhere in the body to the arm. The transferred muscle’s nerve is connected to a working nerve in the arm, and the muscle eventually regains function under new nerve control.
This complex microsurgical procedure requires specialized expertise but can restore grip strength and hand function in otherwise hopeless cases. Recovery takes longer than nerve procedures (12-18 months for functional recovery), but outcomes can be life-changing.
Tendon Transfer
When nerve reconstruction fails or isn’t feasible, tendon transfer procedures reroute working muscles to perform the functions of paralyzed muscles. While not restoring normal nerve function, tendon transfers can restore practical function for daily activities.
Secondary Reconstructive Procedures
Additional procedures addressing residual deficits after primary nerve surgery include shoulder arthrodesis (fusion) for severe shoulder instability, wrist arthrodesis for severe wrist instability, and corrective osteotomies addressing bone deformities from muscle imbalance.
How Top Spine Surgeons in Los Angeles Approach Treatment
Dr. Moksha Ranasinghe’s approach to determining how to treat brachial plexus injury combines comprehensive evaluation, evidence-based decision-making, and personalized treatment planning.
Thorough Diagnostic Evaluation
Evaluation includes detailed history of injury mechanism, comprehensive neurological examination testing each muscle group individually, EMG and nerve conduction studies documenting injury severity and location, and advanced imaging (MRI, CT myelography) identifying nerve root avulsions and structural damage.
Conservative Trial When Appropriate
For injuries with recovery potential, Dr. Ranasinghe recommends appropriate conservative treatment trials while closely monitoring recovery progress. This approach avoids unnecessary surgery while ensuring timely intervention if recovery stalls.
Surgical Expertise When Needed
When surgery becomes necessary, Dr. Ranasinghe’s expertise as a top spine surgeon in Los Angeles encompasses all reconstructive techniques including nerve grafting, nerve transfers, neurolysis, and secondary procedures. Operating at Good Samaritan Hospital and Hollywood Presbyterian Medical Center provides access to advanced microsurgical technology and experienced surgical teams essential for complex nerve reconstruction.
Comprehensive Post-Operative Care
Recovery from brachial plexus surgery requires extensive rehabilitation. Dr. Ranasinghe coordinates closely with specialized hand therapists and occupational therapists experienced in nerve injury rehabilitation, ensuring patients receive optimal post-operative care supporting maximal functional recovery.
Recovery Expectations After Brachial Plexus Treatment
Understanding realistic recovery timelines helps patients maintain appropriate expectations when learning how to treat brachial plexus injury.
Conservative Treatment Recovery
Mild stretch injuries (neurapraxia) typically recover within 3-4 months. More significant nerve damage may require 6-12 months for maximal recovery. Some residual weakness or sensory changes may persist despite good overall recovery.
Surgical Treatment Recovery
Recovery timelines after nerve surgery depend on the procedure performed and distance from nerve repair to target muscles.
Nerve Grafting: Nerve regrows approximately 1mm per day. For a graft connecting to a muscle 200mm away, regrowth takes approximately 200 days (7 months) before functional recovery begins. Total recovery often requires 12-24 months.
Nerve Transfer: Shorter distances mean faster functional recovery, typically 6-12 months depending on the specific transfer performed.
Free Muscle Transfer: Transferred muscles typically show first contractions 3-6 months post-surgery. Functional recovery develops over 12-18 months with continued improvement sometimes occurring up to 24 months.
Factors Affecting Recovery
Patient age (younger patients recover better), injury severity, time between injury and surgery, adherence to rehabilitation protocols, and realistic expectations all influence outcomes. The expertise of the surgical team also significantly impacts results – choosing a top spine surgeon in Los Angeles specializing in brachial plexus reconstruction improves success likelihood substantially.
Why Choose Dr. Ranasinghe for Brachial Plexus Treatment
Patients seeking expertise in how to treat brachial plexus injury choose Dr. Moksha Ranasinghe because she exemplifies the specialized knowledge required for optimal outcomes.
Board Certification and Specialized Training Dr. Ranasinghe is board-certified by the American Board of Neurological Surgery with fellowship training in complex spine surgery and peripheral nerve procedures. This combination provides the nerve reconstruction expertise brachial plexus injuries demand.
Comprehensive Treatment Approach From initial evaluation through long-term rehabilitation, Dr. Ranasinghe provides comprehensive care addressing all aspects of brachial plexus injury treatment. Her conservative-first philosophy ensures surgery is performed only when clinically necessary and appropriately timed.
Advanced Surgical Techniques As a top spine surgeon in Los Angeles, Dr. Ranasinghe performs the full spectrum of brachial plexus reconstruction procedures using microsurgical techniques at major Los Angeles hospitals with experienced surgical teams.
Twenty Years of Experience Two decades of specialized practice treating peripheral nerve injuries provides the experience necessary for optimal decision-making in complex brachial plexus cases.
Frequently Asked Questions
How do doctors determine how to treat brachial plexus injury in individual patients? Treatment decisions depend on injury type (stretch vs. tear vs. avulsion), severity of nerve damage, time since injury, patient age and health, and functional goals. EMG studies and imaging help determine injury severity and recovery potential.
Can all brachial plexus injuries be treated successfully? Mild stretch injuries heal completely in most cases. Severe injuries involving root avulsion have more limited recovery potential, though modern nerve transfer techniques can restore some function. Even with optimal treatment from top spine surgeons in Los Angeles, complete functional restoration isn’t always possible in severe cases.
How long should patients wait before considering surgery? Most specialists recommend waiting 3-6 months to allow spontaneous recovery while monitoring progress. Surgery performed too early risks unnecessary procedures, while surgery delayed beyond 6-12 months allows muscle atrophy limiting recovery potential even with successful nerve repair.
What is the success rate for brachial plexus surgery? Success rates vary by procedure and injury severity. Nerve transfers achieve 80-90% success for restoring critical functions like elbow flexion. Nerve grafting success depends on injury location and graft distance. Free muscle transfers can restore function in carefully selected patients. Choosing experienced surgeons improves outcome likelihood.
How painful is recovery from brachial plexus surgery? Post-operative pain is typically manageable with medications and gradually improves over weeks. The longer-term challenge involves neuropathic pain from the original injury, which requires ongoing pain management regardless of surgical intervention.
Will physical therapy be needed after surgery? Yes, extensive physical therapy is essential after brachial plexus surgery. Therapy prevents contractures during nerve regeneration, rebuilds strength as muscles reinnervate, and maximizes functional outcomes from surgical reconstruction.
Can brachial plexus injuries recur after treatment? Once nerves heal or are surgically repaired, re-injury requires new trauma. However, some patients develop chronic pain or incomplete recovery despite treatment. Regular follow-up with a top spine surgeon in Los Angeles ensures any issues are addressed promptly.
What happens if treatment doesn’t restore adequate function? Secondary procedures including tendon transfers, arthrodesis (joint fusion), or free muscle transfers may provide additional functional improvement. Some patients learn to adapt remarkably well to residual deficits through occupational therapy and assistive devices.
Schedule Your Consultation
If you or someone you know has suffered a brachial plexus injury, prompt evaluation by a specialist is essential. Dr. Moksha Ranasinghe at Southern California Brain and Spine Surgery provides expert assessment of how to treat brachial plexus injury in your specific case, offering both conservative and advanced surgical options.
Call (213) 369-4583 Monday through Friday, 9am to 5pm, or visit socalbrainspine.com to request an appointment.
As a top spine surgeon in Los Angeles with extensive experience in peripheral nerve reconstruction, Dr. Ranasinghe provides the specialized expertise brachial plexus injuries require. Don’t delay evaluation – timing significantly impacts treatment success and functional recovery potential.
- Tags:
- spine diagnosis

